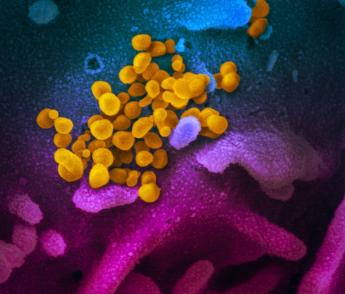
From Off-Guardian:
In a request for a study which shows complete isolation and purification of the particles claimed to be SARS-CoV-2, Michael Laue from one of the world’s most important representatives of the COVID-19 “panicdemic,” the German Robert Koch Institute (RKI), answered that[1]:
I am not aware of a paper which purified isolated SARS-CoV-2.
This is a more than remarkable statement, it is admitting a complete failure. This concession is in line with the statements we presented in our article “COVID-19 PCR Tests Are Scientifically Meaningless” which OffGuardian published on June 27th, 2020 — a piece that was the first one worldwide outlining in detail why SARS-CoV-2 PCR tests are worthless for the diagnosis of a viral infection.
Of course, a line like that should prompt a full reading of the piece. There is more to this story than the lead. And the story is worth reading.
In line with the thread is a perspective published in the New England Journal of Medicine (Mina et al., 2020) from which a no less tantalizing line leads:
It’s time to change how we think about the sensitivity of testing for Covid-19. The Food and Drug Administration (FDA) and the scientific community are currently almost exclusively focused on test sensitivity, a measure of how well an individual assay can detect viral protein or RNA molecules. Critically, this measure neglects the context of how the test is being used. Yet when it comes to the broad screening the United States so desperately needs, context is fundamental. The key question is not how well molecules can be detected in a single sample but how effectively infections can be detected in a population by the repeated use of a given test as part of an overall testing strategy — the sensitivity of the testing regimen.
A similar story by The New York Times reports:
In three sets of testing data that include cycle thresholds, compiled by officials in Massachusetts, New York and Nevada, up to 90 percent of people testing positive carried barely any virus, a review by The Times found.
In addition to false positives reported by RT-PCR tests, there is the question of false negatives. How often does the general class of RT-PCR tests report negative results when the virus may be associated with pneumonia?
Here is Fang et al.,2020:
In our series, the sensitivity of chest CT was greater than that of RT-PCR (98% vs 71%, respectively; P < .001). The reasons for the low efficiency of viral nucleic acid detection may include (a) immature development of nucleic acid detection technology, (b) variation in detection rate from different manufacturers, (c) low patient viral load, or (d) improper clinical sampling. The reasons for the relatively lower detection rate with RT-PCR in our sample compared with a prior report are unknown (3). Our results support the use of chest CT to screen for COVID-19 in patients with clinical and epidemiologic features compatible with COVID-19 infection, particularly when results of RT-PCR tests are negative.
Here is Zitek, 2020:
The sensitivity and specificity of nasopharyngeal swabs using RT-PCR for the diagnosis of COVID-19 cannot be precisely determined with the published data to this point. However, the available in vitro data along with minimal clinical data suggest that the test has very high specificity. On the other hand, the sensitivity is moderate (perhaps between 63–78%). Among the various ways of performing RT-PCR, pharyngeal swabs seem to have lowest sensitivity; nasal swabs may be a bit more sensitive than pharyngeal swabs. RT-PCR analysis of BAL fluid seems to be the most accurate means of virologic confirmation, but BAL fluid can only reasonably be collected on the sickest cohort of patients. For patients with moderate to severe COVID-19 symptoms, identifying characteristic findings on CT imaging of the chest may be more sensitive than RT-PCR testing.
Boger et al., 2021 provides a meta-analysis of CoVid test accuracy considering 16 studies published in April 2020. They assessed a range of tests, including several kinds of PCR tests and observer:
Sixteen studies were evaluated. Meta-analysis showed that computed tomography has high sensitivity (91.9% [89.8%-93.7%]), but low specificity (25.1% [21.0%-29.5%]). The combination of IgM and IgG antibodies demonstrated promising results for both parameters (84.5% [82.2%-86.6%]; 91.6% [86.0%-95.4%], respectively). For RT-PCR tests, rectal stools/swab, urine, and plasma were less sensitive while sputum (97.2% [90.3%-99.7%]) presented higher sensitivity for detecting the virus.
Jaafer et al., 2021 breaks this all down.
It can be observed that at Ct = 25, up to 70% of patients remain positive in culture and that at Ct = 30 this value drops to 20%. At Ct = 35, the value we used to report a positive result for PCR, <3% of cultures are positive. Our Ct value of 35, initially based on the results obtained by RT-PCR on control negative samples in our laboratory and initial results of cultures [8], is validated by the results herein presented and is in correlation with what was proposed in Korea [9] and Taiwan [10]. We could observe that subcultures, especially the first one, allow an increasing percentage of viral isolation in samples with Ct values, confirming that these high Ct values are mostly correlated with low viral loads. From our cohort, we now need to try to understand and define the duration and frequency of live virus shedding in patients on a case-by-case basis in the rare cases when the PCR is positive beyond 10 days, often at a Ct >30.

References:
Böger, B., Fachi, M. M., Vilhena, R. O., Cobre, A. F., Tonin, F. S., & Pontarolo, R. (2021). Systematic review with meta-analysis of the accuracy of diagnostic tests for COVID-19. American Journal of Infection Control, 49(1), 21–29.
Fang, Y., Zhang, H., Xie, J., Lin, M., Ying, L., Pang, P., & Ji, W. (2020). Sensitivity of chest CT for COVID-19: Comparison to RT-PCR. Radiology, 296(2), E115–E117.
Jaafar, R., Aherfi, S., Wurtz, N., Grimaldier, C., Hoang, V. T., Colson, P., … La Scola, B. (2020). Correlation between 3790 qPCR positives samples and positive cell cultures including 1941 SARS-CoV-2 isolates. Clinical Infectious Diseases: An Official Publication of the Infectious Diseases Society of America. doi:10.1093/cid/ciaa1491
Mandavilli, A. (2020, August 29). Your Coronavirus test is positive. Maybe it shouldn’t be. The New York Times. Retrieved from https://www.nytimes.com/2020/08/29/health/coronavirus-testing.html
Mina, M. J., Parker, R., & Larremore, D. B. (2020). Rethinking covid-19 test sensitivity – A strategy for containment. The New England Journal of Medicine, 383(22), e120.
Zitek, T. (2020). The appropriate use of testing for COVID-19. The Western Journal of Emergency Medicine, 21(3), 470–472.
Off-Guardian: